April 15, 2026
Rethinking the fight against antibiotic resistance
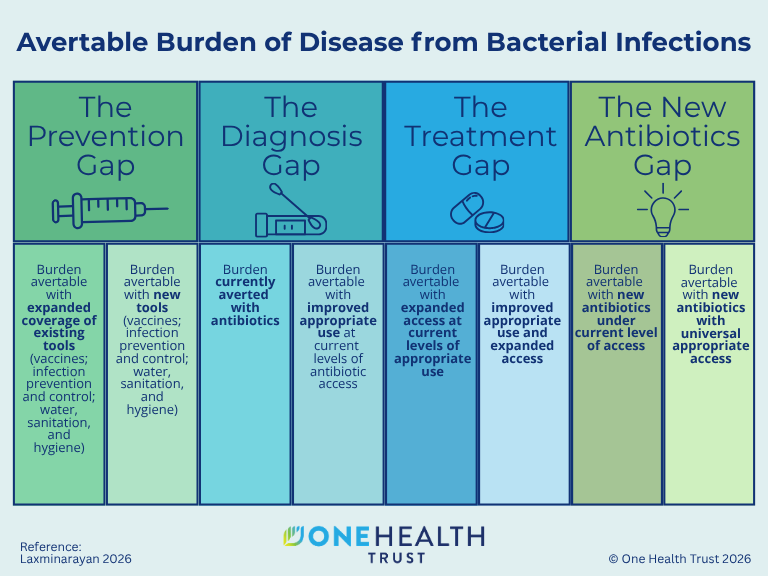
Meeting the United Nations goal of reducing deaths from antibiotic resistance will require more than just developing new drugs. It means rethinking how antibiotics actually reach the people who need them. In the Garrod Lecture, OHT’s Dr. Ramanan Laxminarayan argues that achieving the United Nations General Assembly’s 2024 resolution target of a 10 percent reduction in antibiotic resistance-related deaths by 2030 will require action on 4 fronts: preventing infections through better water, sanitation, and vaccines; improving the use of existing antibiotics; expanding access to effective medicines, especially in low- and middle-income countries; and developing new antibiotics designed for the populations that need them most. Roughly 30 percent of global antibiotic consumption is inappropriate, and nearly 1.4 million serious infections in 8 countries went untreated in 2019 simply because the right drugs were unavailable. Dr. Laxminarayan stresses that too much focus has been placed on new drug development while critical gaps in access to diagnostics and antibiotics remain unaddressed. [Journal of Antimicrobial Chemotherapy]
Why countries should set their own regional health goals
Global development targets like the United Nations Sustainable Development Goals (SDGs) are unlikely to be met by 2030, and the geopolitical framework underpinning them is collapsing. In a new commentary, Dr. Ramanan Laxminarayan and Dr. Olusoji Adeyi argue that countries should focus instead on practical regional development goals developed through bodies such as the African Union and the Association of Southeast Asian Nations. These goals would be financed primarily from domestic resources rather than depending on uncertain foreign aid. With only 35 percent of SDG targets on track, and many regressing below 2015 levels, shifting to regionally driven efforts may be the more realistic path forward. [Nature Health]

How vaccines can help control antibiotic resistance in Kenya
As antimicrobial resistance (AMR) continues to rise around the world, one of the most effective ways to fight it is by preventing infections before they start. Vaccines play a powerful role in that effort. A new policy brief and report from the One Health Trust and the Kenya Medical Research Institute provides practical, Kenya-specific recommendations for using vaccines to reduce antibiotic resistance. By preventing illness, vaccines offer a cost-effective solution to reduce transmission of drug-resistant strains and lower antibiotic use. Despite their significant impact in Kenya, vaccines are still underutilized in the country’s national strategies against AMR. The report calls for increasing vaccine coverage, addressing vaccine hesitancy, and adopting a One Health approach that considers the links between human, animal, and environmental health. [One Health Trust]
New tool reveals how social connections shape epidemic outcomes
Researchers at OHT have created an open-source tool that generates realistic maps of how people interact in cities using publicly available census and commuting data. When researchers ran disease simulations in these networks, they found that accounting for geographic and economic structures reveals clear differences in epidemic spread across neighborhoods, income groups, and racial communities. These insights are often missed by conventional, simpler models. The tool and the synthetic population created are now freely available for other researchers to use and build upon. [Epidemics]

The hidden crisis of antibiotic access in Latin America
While antimicrobial resistance (AMR) is a major source of global mortality, even more people die simply because they cannot get access to the antibiotics they need. In partnership with the South Centre, the One Health Trust launched the policy brief, “Prioritize Antibiotic Access to Tackle Resistance,” in English, Spanish, and Portuguese at the First International Conference on Antimicrobial Resistance in the Americas and Caribbean Region, held in Brasília, Brazil, from March 24–27, 2026. The brief presents evidence on the global consequences of inadequate access to antibiotics, examining key structural, economic, and health system barriers across the region, and shares real-life examples from Latin America illustrating the public health impact of limited antibiotic access. The brief concludes with clear recommendations to ensure people have quick, appropriate, and equitable access to effective antibiotics. [One Health Trust]
Flowing water helps antibiotic resistance spread in rivers exposed to wastewater.
A laboratory study simulating river conditions found that water flow plays a key role in how antibiotic resistance genes accumulate in waterways downstream of wastewater discharge. Microbial communities grown in flowing water maintained higher diversity and sustained or accumulated resistance genes over time, while those in stagnant water progressively lost them. The findings suggest that rivers and streams may be more effective than still water bodies at harboring and spreading resistance genes introduced by wastewater, and water flow should be carefully considered in environmental monitoring and wastewater management efforts. [Microbial Ecology]
Challenges in Senegal’s effort to fight antibiotic resistance
Senegal has made progress by creating a national platform in 2017 to coordinate efforts against antibiotic resistance across human, animal, and environmental health. However, a new study based on interviews with key stakeholders shows that the platform’s effectiveness is undermined by weak legal authority, a lack of domestic funding, and heavy reliance on international donors. Outdated regulations still allow antibiotics to be dispensed without prescriptions, and rural areas lack the laboratory infrastructure needed to guide appropriate prescribing and track resistance. The researchers call for stronger legal frameworks, greater domestic investment, and more inclusive policymaking that connects global standards with local realities. [PLOS Global Public Health]
Climate-related disasters are increasing infectious disease risks in eastern Uganda.
In eastern Uganda, extreme weather events such as floods, landslides, and droughts are making certain infectious diseases more common. A new study found that in the affected districts, malaria was nearly twice as common, diarrheal illnesses were 1.2 times more common, and typhoid fever was up to 90 times more common than the national average. Floods were linked to a higher risk across all three diseases, while droughts and landslides particularly increased the risk of diarrheal illnesses. These trends show how environmental disturbances impact vector habitats, sanitation, and water quality and highlight the need for better water and sanitation infrastructure, targeted health measures in vulnerable areas, and stronger climate adaptation efforts. [Discover Environment]
Explainable AI can improve One Health approaches to controlling infectious disease.
New research shows how “explainable” artificial intelligence (AI) can improve prevention and control of infectious diseases within a One Health framework. With over 60 percent of infectious diseases coming from zoonotic sources, understanding the links between human, animal, and environmental systems is more important than ever. Explainable AI enhances conventional modeling by pinpointing important epidemic drivers and providing forecasts that decision-makers can understand and trust. While challenges remain around data quality and interpretation, the approach holds promise for better surveillance, resource allocation, and predicting disease spillover. [eBioMedicine]
How colonial legacies still affect public health in India
Many of India’s current public health laws, such as the Epidemic Diseases Act and pharmaceutical laws, were originally designed during British colonial rule to protect trade and maintain control rather than improve people’s health. In his column, Vital Signs, Dr. Ramanan Laxminarayan explains how these enduring colonial structures continue to shape India’s public health system today. He also notes lasting regional disparities: formerly British-ruled areas continue to have higher rates of infant mortality and poverty, while regions that made larger early investments in health and education, especially in southern India, show better outcomes. Dr. Laxminarayan argues that real progress will require moving beyond inherited frameworks, toward equitable, people-centered health systems. [Hindustan Times]