June 24, 2017
Commonly known as a “Superbug,” methicillin-resistant Staphylococcus aureus (MRSA) is a frequent cause of infection in hospital and community settings. MRSA is resistant to many conventional antibiotic treatments making management of these infections particularly difficult. Because of MRSA’s ubiquitous presence and its changing epidemiology, it is a very important and challenging antibiotic-resistant pathogen.
Trends in Methicillin-Resistant Staphylococcus Aureus Infections
CDDEP’s work on MRSA has examined trends in the burden of MRSA infections in the United States, finding that hospitalization rates for MRSA-related skin and soft-tissue infections (SSTIs) decreased between 2010 and 2014, while rates for more invasive MRSA-related infections, sepsis, remained constant.
MRSA is the leading cause of mortality due to antibiotic-resistant infections in the United States. Rates of MRSA remain higher in the United States than in most other developed countries, particularly for invasive sepsis and pneumonia, which are often transmitted in hospitals.
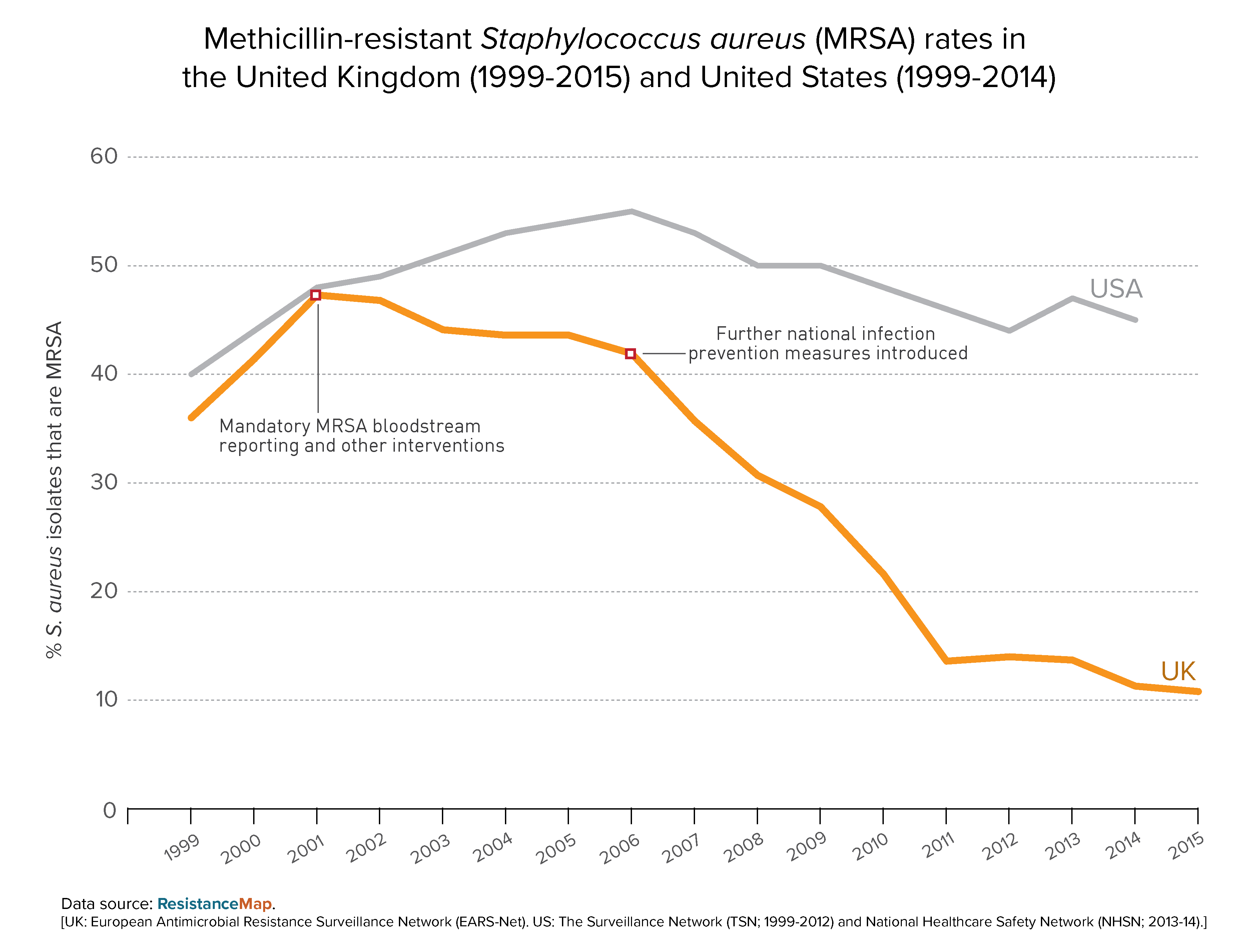
The arc of MRSA prevalence in the United Kingdom illustrates the power of public policy interventions to slow the spread of antibiotic-resistant bacteria. Depicted in this graphic generated from CDDEP’s ResistanceMap, the rising rate of MRSA bloodstream infections (BSIs), which peaked at 47 percent in 2001 and 2002, led to the introduction of new policies intended to control it.
Following the implementation of infection prevention measures, MRSA resistance rates fell dramatically. Contrast this with MRSA’s trajectory in the United States, which took no definitive steps to either recognize the rising tide of MRSA or to change practices to control it.