March 25, 2013
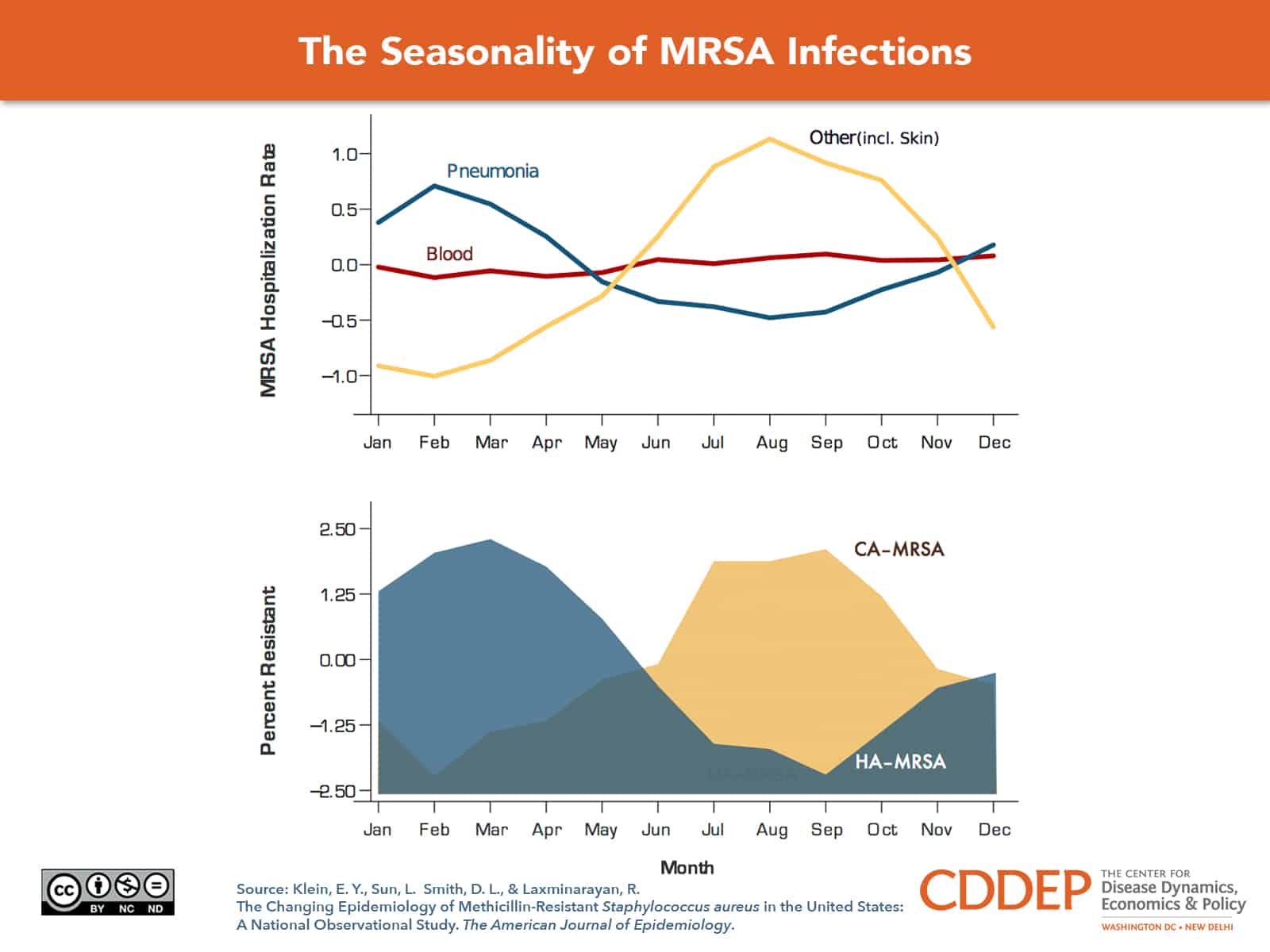
Normally found on human skin, Staphylococcus aureus can infect wounds and cause life-threatening conditions such as sepsis and pneumonia. Strains of methicillin-resistant S. aureus (MRSA) fail to respond to commonly used antibiotics, making infections more expensive and difficult to treat. The early 2000s were marked by the rapid emergence of community-associated strains (CA-MRSA) and their move into hospitals, where they only added to the existing burden of healthcare-associated strains (HA-MRSA).
Most recently, Klein et al found that CA and HA infections show different seasonal and age patterns. The graph shows the seasonal peaks of hospitalizations by infection site (top panel) and prevalence of each subtype of MRSA (bottom panel). The community-associated MRSA strains, which primarily affect younger populations, tend to cause skin infections and peak in the summer months. Hospital strains, affect older populations, have a winter peak which coincides with a lull in MRSA-related pneumonia hosptializations. The winter low in community infections could be driven by antibiotic usage for other indications, which hits a high in winter flu season and is higher in children.