Overview
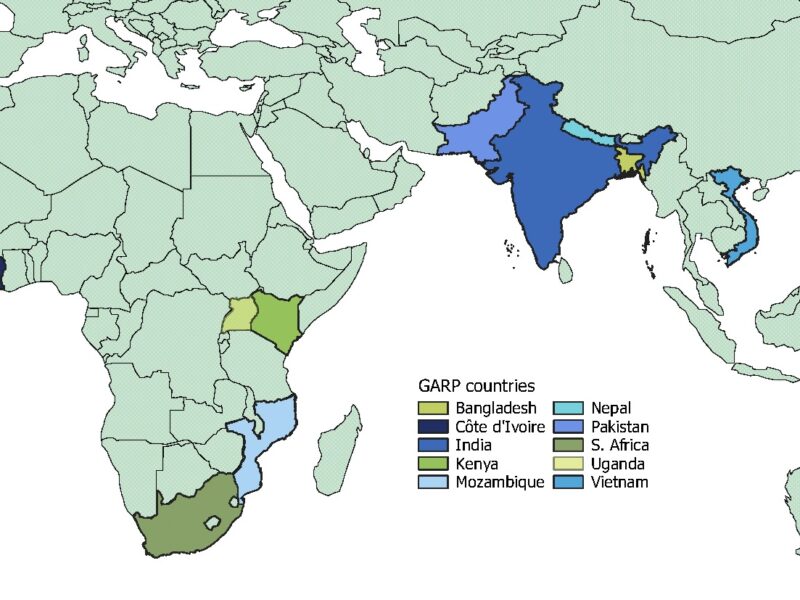
Each year between 2008 and 2012, India had an estimated 675,000 cholera cases and 20,000 cholera deaths. The year 2016 saw 6.2 million typhoid cases and 66,400 typhoid-associated deaths, with 10,200 deaths among children under five. Despite this enormous health burden, India’s Universal Immunization Program does not include cholera or typhoid vaccines for children. To inform India’s vaccination policy, One Health Trust researchers have estimated the cost-effectiveness of delivering typhoid and cholera vaccines to children under five.
The Study
OHT researchers estimated the reductions in health burden and economic cost from cholera and typhoid vaccination among children under five. Using parameters from published sources and employing a static Markov model over five years, researchers estimated the incident cases, deaths, disability-adjusted life years (DALYs), hospitalization costs, outpatient visit costs averted, and economic benefits from mortality risk reduction under two scenarios:
- introduction of cholera and typhoid vaccines at current complete immunization rates; and
- scaling up cholera and typhoid vaccine coverage to 90 percent.
The highest benefits from vaccination were estimated to be among children in the lowest wealth quintile and poorer Indian states. The incremental cost-effectiveness of both scenarios would be approximately US$108 per DALY averted, with benefit-cost ratios greater than one.
For policymakers, public health interventions are generally considered cost-effective if the incremental cost-effectiveness ratio is less than one-third of gross domestic product (GDP) per capita. With a GDP per capita in 2020 of US$1,900 and an incremental cost-effectiveness ratio of approximately US$108, both typhoid and cholera vaccinations for young children would be highly cost-effective.
Funding
The Bill and Melinda Gates Foundation